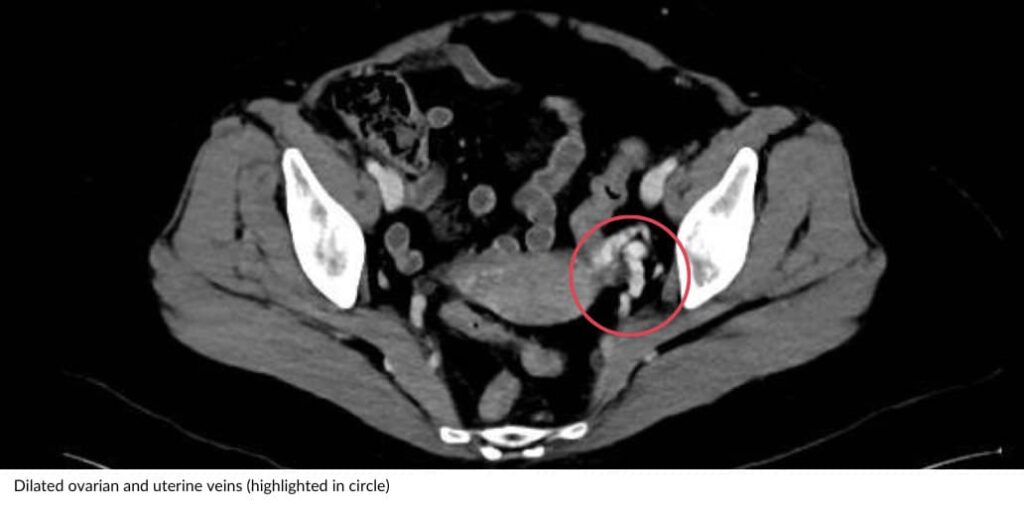
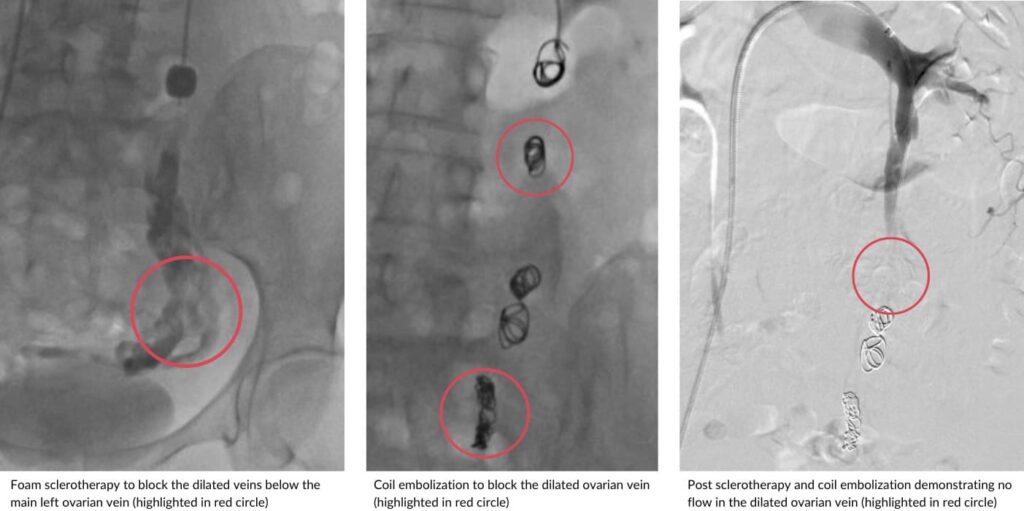
Pelvic congestion syndrome is caused by enlarged pelvic veins that pool blood and trigger ongoing pelvic pain. Symptoms may worsen after standing, during periods, or after sex. Assessment uses scans to confirm vein reflux. Treatment ranges from medication to minimally invasive vein embolisation to close faulty veins and relieve pressure.