What is Venous Disease?
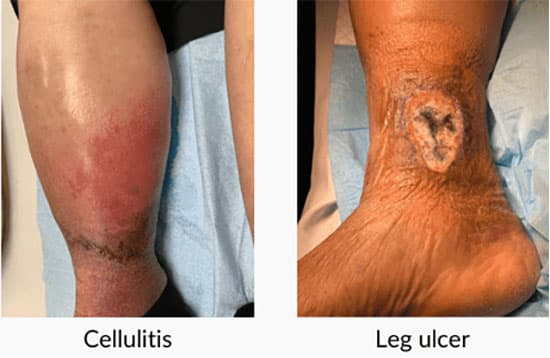
Chronic venous insufficiency (CVI) is a common condition that occurs when the wall and/ or the valves of the veins in your legs do not work properly, making it difficult for blood to return efficiently from the legs back to the heart.
Normally, the valves on the leg veins ensure that blood flows towards your heart in a one-way system but when they don’t work well, blood can also flow backwards and collect in the legs, causing venous stasis.