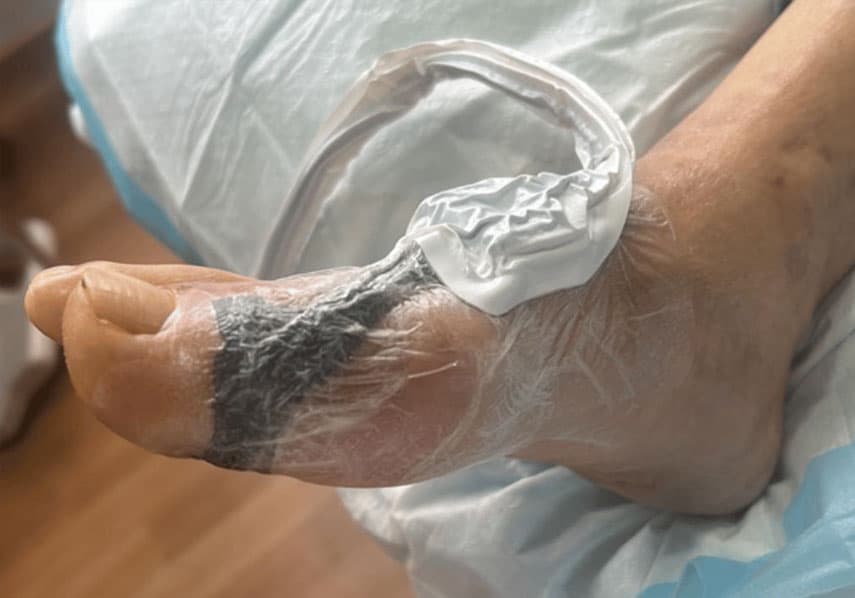
Vacuum-assisted closure (VAC) is a type of wound therapy that involves using a specialised device to create negative pressure or suction around and on a wound. The device consists of a foam dressing that is placed over the wound and then covered with a transparent film. A tube is then connected to the device, which creates a vacuum, drawing out excess fluid and promoting blood flow to the wound.
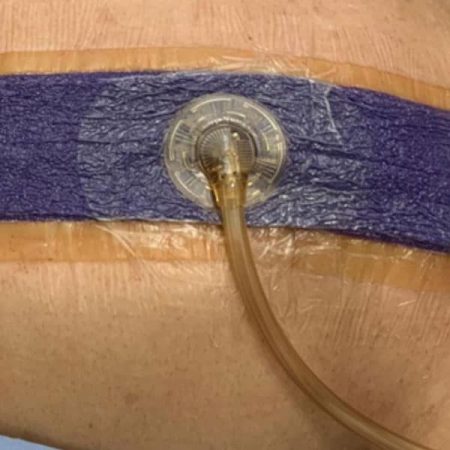
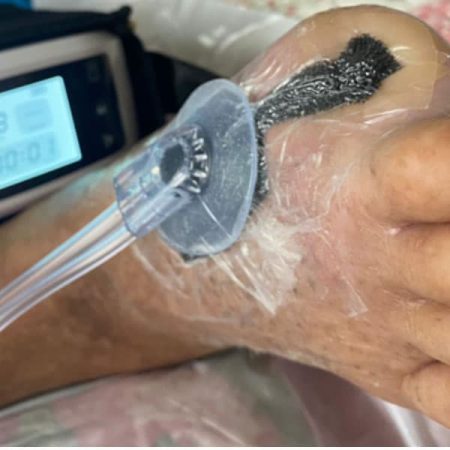
Vacuum-assisted closure therapy is used to help treat chronic, non-healing wounds, such as diabetic ulcers, pressure ulcers, and surgical wounds. The negative pressure helps to remove excess fluid and debris, which can reduce swelling, decrease the risk of infection, and promote faster healing. Vacuum-assisted closure therapy is typically performed in a medical setting, such as a hospital or wound care center, under the supervision of a healthcare professional. It may be used in conjunction with other treatments, such as antibiotics and debridement, to help facilitate wound healing.
The benefits of using vacuum-assisted closure for wound therapy include:
- Faster healing: VAC therapy has been shown to promote faster wound healing by increasing blood flow and oxygenation to the wound bed.
- Reduced risk of infection: The negative pressure created by the VAC device helps to remove excess fluid and debris from the wound, which can help reduce the risk of infection.
- Improved wound bed preparation: VAC therapy can help prepare the wound bed for other treatments, such as skin grafts or surgical closure, by removing excess fluid and promoting healthy tissue growth.
- Increased patient comfort: VAC therapy can help reduce pain and discomfort associated with chronic wounds by promoting faster healing and reducing swelling.
- Cost-effective: VAC therapy has been shown to be cost-effective compared to other wound therapies, as it can reduce the need for hospitalization and other medical interventions.
Vacuum-assisted closure therapy can cause some discomfort and pain, especially during the first few days of treatment. However, patients are usually given pain medication to help manage the pain. It is important to communicate any pain or discomfort to your healthcare provider so they can adjust the treatment as needed.
Living with the Vacuum-Assisted Closure Device
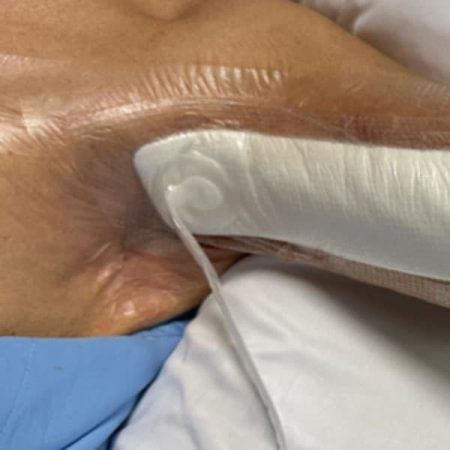
Patients can usually sleep with the vacuum-assisted closure device on, as it is designed to be worn continuously. However, it may take some time to adjust to the feeling of the device and the noise it makes. Your healthcare provider can provide tips on how to manage any discomfort or difficulty sleeping with the vacuum-assisted closure device on.
Walking with a vacuum-assisted closure device may be possible, depending on the location and size of the wound being treated. However, it is important to follow the instructions of your healthcare provider regarding activity and movement while using the vacuum-assisted closure device.
In some cases, it may be necessary to limit physical activity or immobilize the affected area to allow for proper healing and treatment. Your healthcare provider can provide specific instructions on how to care for the wound and use the vacuum-assisted closure device while still engaging in daily activities.
The length of time that you will need to use the vacuum-assisted closure device will vary based on the specific wound and your response to treatment. Your healthcare provider will monitor your progress and determine when it is appropriate to discontinue the use of the VAC device and transition to other forms of wound care.
It’s important to follow your healthcare provider’s instructions for wound care and use of the VAC device to ensure the best possible outcome for your wound healing.
There are different types of vacuum-assisted closure (VAC) devices, including:
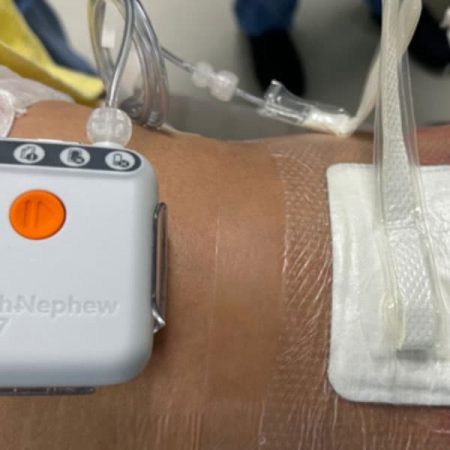
- Portable VACs: These are lightweight and portable devices that are used for small or relatively shallow wounds. They are often used in home care settings and can be worn on a belt or carried in a small bag.
- Stationary VACs: These are larger devices that are used for larger or deeper wounds. They are typically used in hospital settings or other medical facilities. They may be attached to a bedside stand or cart.
- Disposable VACs: These devices are designed for single use and are often used in surgical settings. They are lightweight and portable and can be discarded after use.
- Negative pressure wound therapy (NPWT) with instillation is a type of advanced wound care that combines the use of negative pressure to promote healing with the instillation of a topical wound solution. The wound is first cleaned and then a wound dressing is applied. A specialized NPWT device is then attached to the dressing, creating a vacuum that helps to remove excess fluid and bacteria from the wound. In addition to the negative pressure, a wound solution is instilled into the wound bed through special channels in the dressing. The solution can help to dissolve debris and bacteria, promote tissue growth, and improve wound healing. This combined approach of negative pressure and instillation can be particularly effective for wounds that are difficult to heal, such as those with high levels of exudate (fluid). However, NPWT with instillation is a specialized treatment that requires proper training and experience to administer safely and effectively. It is typically performed by healthcare professionals in a hospital or clinic setting.
The specific type of VAC device used will depend on the type and severity of the wound, as well as other factors such as the patient’s mobility and treatment setting. Your healthcare provider will determine which type of VAC device is most appropriate for your wound and treatment needs.
Overall, VAC therapy is a safe and effective treatment option for chronic wounds and has been shown to improve patient outcomes and reduce healthcare costs.